
05 Aug To Your Health: A Few Pointers on Ticks + 8 Dangerous Bugs To Avoid
Dr. Alan Safdi, a world-renowned internist and gastroenterologist with encyclopedic knowledge of mind-body wellness and preventative medicine, posts on Telluride Inside… and Out under the banner of “To Your Health.” His blogs feature the most current information in his field: health, wellness, and longevity.
This fall, Dr. Alan returns with his popular Live Longer Retreat wellness intensives. For further information, email telluridecme@gmail.com. or go to Safdi’s Telluride Longevity Institute website.
This week, Dr. Alan talks about ticks and 8 dangerous bugs to avoid.
And here is a link to a recent New Yorker article titled “Bloodsucking Parasite Dept. Tickbusters. Apparently the black-legged tick problem in and around New York is growing threat.
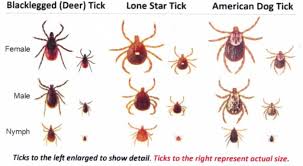
First a few pointers about ticks.
While burning a tick off the skin may seem like a satisfying and fool-proof way to get the blood-sucker off, it’s also the worst way to remove it.
Burning it may actually increase the risk of getting a tick-borne disease.
Applying heat can increase [the tick’s] saliva production and, if it’s infected with something nasty, increase pathogen transmission. The best way to remove a tick is to use tweezers and grab the tick as close to the skin as possible and pull straight out. Ticks can’t jump; they lack the biomechanics to do that. Ticks crawl from one part of your body to the next.
Rocky Mountain spotted fever is a tick-borne illness caused by the bacteria Rickettsia rickettsii. It is potentially fatal in humans and is transmitted in the U.S. by bites from the American dog tick, Rocky Mountain wood tick, and brown dog tick, according to the Centers for Disease Control and Prevention.
Powassan is a potentially fatal virus transmitted by tick bites. Powassan can be fatal, and some of those who survive may have long-term neurological damage. There are no treatments.
When it comes to Lyme disease and all tick-related bites, people should be vigilant about checking their bodies and if a tick is found remove it quickly.
Ticks must be attached to humans for 36 to 48 hours or more before the Lyme bacteria can be transmitted.
The CDC said that some 96,075 diseases caused by bites by mosquitoes, ticks, and fleas were reported in 2016, up from 27,388 in 2004, in an analysis of data from the CDC’s National Notifiable Diseases Surveillance System. In essence, we are seeing a very significant increase in these diseases from mosquitoes and ticks.
So what symptoms or signs should you look for with some of these diseases?
Rocky Mountain spotted fever (RMSF) is a potentially lethal, but curable tick-borne disease, first described in Idaho in the 19th century. The classic clinical triad of fever, headache, and rash may be present in less than 5% of patients in the first 3 days of illness, but increases to 60-70% by the second week after tick exposure. The absence or delayed appearance of a rash increases the difficulty of diagnosis.
The most common symptom complaints include the following:
Fever greater than 102°F – 94% of reported cases
Fever within three days after tick bite – 66% of reported cases
Headache, frequently severe – 86% of reported cases
Myalgias – 85% of reported cases
CNS symptoms – 25% of patients develop signs of encephalitis (i.e., confusion, lethargy); this may progress to stupor, delirium, seizures, or coma
GI symptoms – Some patients present with anorexia, nausea, vomiting, diarrhea, and abdominal pain
RMSF should be considered in patients with unexplained febrile illness even if they have no history of a tick bite or have travelled to an endemic area. The history of a tick bite is reported by only 70% of patients. (Most tick bites are painless and may be in hidden areas of the body.)
Lyme disease
Lyme disease has a broad spectrum of clinical manifestations. It also varies in severity due, in part, to differences in the infecting species. Lyme disease was first described in 1977 as “Lyme arthritis” in studies of a cluster in Connecticut of children thought to have juvenile rheumatoid arthritis.
Physical findings in patients with early disease are as follows:
Flulike illness – Fever, chills, malaise, myalgias (muscle aches), arthralgia (painful joints), headache
Tender local adenopathy (lymph nodes) (local, not diffuse)
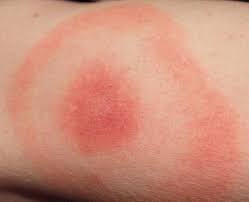
Erythema migrans (EM) – Rash
This is similar to a bull’s eye rash seen in early Lyme disease:
Insects in general:

Look out for more and increasingly dangerous insect encounters this summer. With the erratic winter and spring weather patterns we’ve had across the country—deep snows, driving rains and widespread flooding—this could be a bad year for insect-borne illnesses. Standing water is a breeding ground for mosquitoes, for instance, and the flooding and rainfall in the Midwest this spring has led to an increased number of breeding sites.
Illnesses from mosquito bites, along with bites from ticks and fleas, have tripled in the United States in the past 15 years.
“The data show that we’re seeing a steady increase and spread of tick-borne diseases, and an accelerating trend of mosquito-borne diseases introduced from other parts of the world,” said Lyle Petersen, MD, MPH, director, Division of Vector-Borne Diseases, CDC National Center for Emerging and Zoonotic Infectious Diseases.
Notable insect-borne infections include West Nile virus, dengue fever, Zika virus, Lyme disease, chikungunya, ehrlichiosis, and anaplasmosis. But disease-carrying mosquitoes, ticks, and fleas aren’t the only dangers lurking in your backyard or near your campground.
Killer bee:

Honey bees, as you’ve probably heard, are in danger. But Africanized honey bees (commonly called “killer bees”) are a danger, having caused the deaths of more than 1,000 people worldwide. Africanized bees look like average honey bees, but are a hybrid strain that can get extremely defensive to the point of aggression—they can chase people for more than a quarter of a mile. Although their stings are no worse than those of typical honey bees, killer bees attack in swarms, resulting in hundreds or thousands of stings. Killer bees have colonized in Texas, Arizona, Nevada, New Mexico, Florida, California, Louisiana, and Arkansas. They continue to move northward.
Kissing bug:

Triatomine bugs—more commonly called “kissing bugs” because they tend to bite victims around the mouth or eyes while asleep—are now found in 28 states, particularly in Southern states. Approximately 50% of these nocturnal bloodsuckers carry a parasite (Trypanosoma cruzi), which they pass to humans, dogs, rodents, and other mammals that they bite. Humans or animals infected with this parasite have about a 30% risk of developing chronic Chagas disease, which can lead to cardiac and/or intestinal complications even years later.
Lone Star tick:

Named after the white, star-like splotch on its back, the Lone Star tick (Ambylomma americanum) is a very aggressive, human-biting insect. Found primarily in the Southern and Eastern states, the Lone Star tick can cause infection that can lead to a number of conditions—one of which is alpha-gal allergy, a severe reaction to eating meat.
“It’s a case of cruel irony indeed that a tick named after Texas can render you unable to eat red meat,” observed the author of a Popular Science article. Other diseases caused by infection from the Lone Star tick include ehrlichiosis, Heartland virus, Southern tick-associated rash illness (STARI), and tularemia.
The Lone Star tick has also been linked to the newly discovered Bourbon virus, a disease that appears similar to ehrlichiosis, but with no known treatment. The disease was named after the first-known fatal victim’s home county of Bourbon, KS. But people in Northern states aren’t necessarily immune: warming temperatures are making a comfortable climate throughout the nation for this aggressive species.
Yellow sac spider:

Yellow sac spiders are one of the most aggressive spiders in North America, often biting without provocation. They’re probably responsible for more human bites than any other species of spider. Rather than waiting in their sac-like webs, they roam about in search of prey. Their bite causes a burning pain that can last up to an hour, along with redness, swelling, and itching, followed by a rash and blistering. Yellow sac spiders have been commonly found in New England and the Midwest, but their range has likely increased over time, spreading throughout most of the United States.
Arizona bark scorpion:

The Arizona bark scorpion is the most venomous scorpion in North America—the only native scorpion considered to be life-threatening. Its sting can cause excruciating pain, numbness, tingling, and vomiting. Although it dwells throughout Arizona (as its name implies), the bark scorpion is found from southern California into western New Mexico. It’s a good climber and can be found in between rocks, in trees, or high on rock walls—but also in houses: in a sink or bathtub, a dark closet, or climbing up a wall. They hide during the day to avoid the heat, but come out in the cool of the night to hunt.
Brown recluse spider:

These harmless-looking brown spiders like to stay hidden in small dark areas, but bites from these venomous arachnids are believed to rise during summer months, perhaps because people rouse them from the dark corners of garages, basements, attics, and yards.
The brown recluse is found in 15 states, chiefly in the South and Southwest. Their venom is known to be extremely painful. The bite wound usually reddens within several hours. This is followed by a systemic reaction within 24-36 hours, characterized by restlessness, fever, chills, nausea, weakness, joint pain and, in rare cases, convulsions and death. The bite wound and the surrounding tissue can blacken, die, and eventually shed.
Deer tick:

Also known as black-legged ticks (Ixodes scapularis), deer ticks carry Lyme disease and other infections—and are now found even in America’s largest cities. While frequently reported in New England, Lyme disease carried by deer ticks also occurs in Eastern and Midwestern states, and coastal California; however, Lyme has been reported in nearly every state. Deer ticks also transmit pathogens that cause anaplasmosis, ehrlichiosis, babesiosis, and the rare, but deadly Powassan virus mentioned above.
And their territory is expanding—the number of counties in which deer ticks are now established has more than doubled in the past 20 years.
Mosquito:

Mosquitoes cause more human suffering than any other organism, with more than 1 million people worldwide dying from mosquito-borne diseases each year, according to the American Mosquito Control Association.
Mosquitoes not only cause annoying summertime itches, but they also spread malaria, West Nile virus, Zika virus, dengue fever, yellow fever, and St. Louis encephalitis. Every state harbors some sort of disease-carrying mosquito. Malaria-carrying mosquitoes are found in the Southern and Eastern states as well as in coastal California. Mosquitoes carrying West Nile virus may appear in flood-ravaged Midwestern states this summer. Dengue fever has occurred in Florida and Puerto Rico, and cases of dengue are expected to rise and spread to more states in coming years.
Don’t let this article disturb. Knowledge is always a good thing. So, in short, don’t forget your insect repellent this summer!
Dr. Alan, more:

Dr. Alan Safdi is board-certified in Internal Medicine and in Gastroenterology and is a Fellow of the American College of Gastroenterology. A proven leader in the healthcare arena, he has been featured on the national program, “Medical Crossfire” and authored or co-authored numerous medical articles and abstracts. Safdi has been involved in grant-based and clinical research for 30+ years and is passionate about disease prevention and wellness, not just fixing what has gone wrong. He is an international lecturer on the subjects of wellness, nutrition and gastroenterology.
And back by popular demand, this summer, in partnership with the Peaks’ Spa, Dr. Safdi returns with his three, week-long wellness intensives titled Live Longer Retreat.
Again, using an evidence-based, scientific approach to health and longevity and featuring an experienced staff of medical professionals, personal trainers, Pilates and yoga instructors, dietitians, and chefs, the focus is on your unique wellness profile. Each Live Longer Retreat is one-of-kind in the U.S. Those intensives, limited to only 10 – 15 participants, will include personal consultations, hiking, spinning, yoga, Pilates, talks and demonstrations related to nutrition, cooking classes, and more.
Go here to read a review of the experience by one very satisfied participant.
Feel free to sign up now to participate in a Live Longer Retreat – or call 1-877-448-5416 for further information.


Sorry, the comment form is closed at this time.